Table of contentIn this article
- When adults should see a doctor for an eye infection
- When to take your child to see a doctor for an eye infection
- Signs it’s time to see a doctor for an eye infection
- Types of eye infections
- High-risk groups for eye infections
- How doctors treat eye infections
- How Doctor On Demand can help with your eye infection
- Doctor-answered eye infection FAQs
Have red, itchy eyes or blurry vision? Eye infections are common, and some are serious. Here’s how to know when it’s simply irritation or when to see a doctor, and what kind of doctor. Learn the warning signs, treatment options, and the care needed.
When adults should see a doctor for an eye infection
Eye infections are common, but some need a doctor’s care. Redness, pain, swelling, or thick discharge can be signs of a serious problem. If your vision changes or symptoms don’t improve in a day or two, it’s time to see a doctor. Fast care can help protect your sight.
A 2010 American Family Physician article, “Diagnosis and Management of Red Eye in Primary Care,” notes that red eye, or ocular inflammation, is one of the most common eye conditions for which people see a doctor. The authors write, “Ocular inflammation of almost any part of the eye, including the lacrimal glands and eyelids, or faulty tear film can lead to red eye. Primary care physicians often effectively manage red eye, although knowing when to refer patients to an ophthalmologist is crucial.”
When is an eye infection an emergency?
An eye infection is an emergency if you have sudden vision loss, severe pain, chemical exposure, an eye injury, or eye symptoms accompanied by fever, nausea, or vomiting, which may indicate a spreading infection or a more serious condition like meningitis.
An eye infection may be an emergency if you have any of the following:
- Severe eye pain: This could mean a serious problem inside the eye, like inflammation or a deep infection, which could lead to vision loss.
- Sudden vision loss or significant vision changes: Losing vision quickly or seeing blurry or dark spots could indicate a severe eye disease that needs fast treatment.
- Swelling around the eye that spreads to the cheek or forehead: Swelling might indicate orbital cellulitis, a dangerous infection that can spread and affect your brain or eyesight.
- Bulging of the eye: If your eye looks like it’s sticking out, it may be due to pressure behind the eye caused by infection or swelling.
- High fever with eye symptoms: A fever and red, painful, or swollen eyes may mean the infection is spreading and needs emergency care.
- Trouble moving the eye or seeing double: If you can’t move your eye normally or see two of everything, an infection may be affecting your eye muscles or nerves.
- Recent eye surgery or injury with redness, discharge, or pain: These symptoms may be signs of an infection that could damage the eye quickly after surgery or an injury.
- Pus-like discharge that gets worse fast: Thick, yellow, or green discharge that increases quickly can indicate a fast-moving bacterial infection.
- Light sensitivity with headaches or a stiff neck: Being very sensitive to light, along with a stiff neck or headache, may be a sign of a serious infection like meningitis.
When to use urgent care for an eye infection
You can use urgent care for non-emergency eye infections. Go to urgent care if you have persistent eye redness or discharge that doesn’t improve with treatment, and mild to moderate pain with no vision changes. Bacterial conjunctivitis, common among contact lens wearers, is treatable at urgent care.
Here are the signs that you should visit an urgent care clinic:
- Eye redness and swelling that’s getting worse: This is a sign that could mean the infection is spreading or not healing.
- Mild to moderate eye pain: Urgent care can help find the cause and start treatment.
- Sticky or colored eye discharge: Yellow or green mucus may indicate bacterial infection.
- Itchy, watery eyes that don’t improve: This could be viral or allergic conjunctivitis that needs treatment.
- There have been no vision changes, but symptoms have not improved after a few days: If home care isn’t working, it’s time to get checked.
- You wear contact lenses and notice irritation or redness: Contact lens users are at higher risk for infections.
- You’re unsure what type of infection it is: Urgent care can help determine whether it’s viral, bacterial, or something else.
Urgent care is a good choice when your symptoms are not severe enough for the ER but still need quick attention. They can treat most common eye infections and refer you to a specialist.
When to use telehealth for an eye infection
Telehealth can be used for an eye infection if your symptoms are mild to moderate. It’s a good choice if you have redness, itching, mild swelling, watery or sticky discharge, or mild pain. However, in-person care works best for vision changes, severe pain, or worsening symptoms.
If your symptoms are mild and you don’t need hands-on care, a telehealth visit can be a safe and convenient way to get help. Here’s when telehealth makes sense:
- Red or itchy eyes without severe pain: A doctor can evaluate these symptoms by video and recommend treatment.
- Transparent or slightly sticky discharge: If the discharge isn’t thick or green, you may have a mild viral or allergic infection.
- Mild eyelid swelling: A video call can help decide if medicine is needed or if a doctor should see you in person.
- Symptoms are not getting worse: If things are staying the same but not improving, telehealth can help guide next steps.
- You need a prescription or advice: A telehealth doctor can prescribe eye drops or suggest over-the-counter care.
- You want to know if it’s contagious. A virtual visit can help confirm the type of infection and teach you how to avoid spreading it.
Telehealth is a smart first step for mild eye infections. If the provider sees signs of something more serious, they’ll tell you to visit urgent care or see an eye doctor.
When to see an ophthalmologist for an eye infection
See an ophthalmologist if your eye infection doesn’t improve with treatment or affects your vision, or if you’re in a high-risk group. This includes contact lens wearers, people with a weakened immune system, and newborns under one month old. A specialist can check for serious problems and provide care.
If you have sudden vision changes or loss, severe or ongoing pain, or an eye injury, visit an ophthalmologist. These specialists treat disorders and diseases of the eye. Other reasons include signs of infection that don’t improve, like redness, swelling, or discharge. You should also go to an ophthamologist if you see flashes of light, floaters, or a shadow in your vision, have dry eyes that won’t go away, have double vision, or have trouble seeing at night. People with contact lens problems, past eye surgery, diabetes, or a family history of eye diseases like glaucoma should also get checked regularly.
People with advanced HIV, especially those with low CD4 counts, are at higher risk for serious eye infections like CMV retinitis. If any eye symptoms appear, they should be referred to an ophthalmologist promptly.
Doctors should immediately examine premature and newborn babies who have severe symptoms, signs of an eye infection, or a family history of conditions that affect the eyes.
When to see your primary care doctor for an eye infection
If your eye is red, itchy, swollen, or has mild discharge, see your primary care doctor. They can check for common problems, start treatment, and tell you if you need to see a specialist.
Some non-infectious, mild eye conditions may go away on their own. However, your primary care doctor can provide medical advice and treatment if they don’t. Your doctor may refer you to an ophthalmologist if symptoms worsen after initial treatment.
Eye conditions that can be mistaken for infections
Some eye conditions, like allergies, blocked glands, or irritation, can look like infections. These problems need different treatments, so knowing the difference is essential. This guide helps you spot common eye issues people often mistake for infections and explains when to see a doctor for care.
Here’s a list of common eye issues that initially may mimic infections, and when to talk to your doctor:
- Allergic conjunctivitis: Red, itchy, and watery eyes are the main symptoms of allergic conjunctivitis, sometimes called allergic pink eye. It can be mistaken for viral or bacterial conjunctivitis, which are contagious forms of pink eye. Allergic conjunctivitis is not contagious and usually improves with allergy medicine or antihistamine eye drops.
- Chalazion: A painless lump from a blocked oil gland. Use warm compresses several times a day to help it drain. If it doesn’t go away, a doctor may prescribe medicine or drain it.
- Dry eye syndrome: The eyes feel dry or gritty because they lack natural tears. For relief, use eye drops or artificial tears. Avoid dry air and take breaks from screens. Severe cases may need prescription drops.
- Eye floaters: Small spots or lines in vision, common with aging. Most floaters are harmless and don’t need treatment. See an eye doctor if they suddenly increase or come with light flashes.
- Blepharospasm: Uncontrolled blinking or eyelid twitching, often temporary. Try resting and reducing stress. A doctor might recommend Botox shots to relax the muscles if twitching continues.
- Pterygium: A non-cancerous growth on the white of the eye from sun or dust exposure. Wear sunglasses and avoid dust or wind. Use eye drops for comfort. If the pterygium enlarges or affects vision, surgery is the recommended course of treatment.
- Subconjunctival hemorrhage: A red spot from a burst blood vessel, usually harmless. No treatment is needed. The red spot goes away in 1–2 weeks. See a doctor if it happens often or comes with pain.
Even though these symptoms are mostly benign, you should see an eye care professional to ensure you don’t have a severe infection, or if the doctor recommends something that will bring relief. At the same time, you wait for the condition to resolve.
When to take your child to see a doctor for an eye infection
Take your child to the doctor if they have red eyes, swelling, yellow or green discharge, or eye pain. See a doctor immediately if the infection doesn’t get better in a few days, worsens, or if your child is a baby under one month old. Early care helps prevent problems.
Eye infections in children range from mild to serious. While some clear up on their own, others can damage vision if left untreated. Getting timely care is especially important in newborns and infants, where symptoms can escalate quickly.
A 2023 study, “Pediatric Conjunctivitis: A Review of Clinical Manifestations, Diagnosis, and Management,” found that bacteria cause most eye infections in children. Viral conjunctivitis often happens with colds or the flu, while allergic conjunctivitis usually affects both eyes during allergy season when pollen levels are high.
While most cases are not critical, having a physician examine your child if they have persistent symptoms is the most sensible thing to do.
When to take your newborn to see a doctor for an eye infection
Take your newborn to the doctor immediately if you see red eyes, swelling, or any eye discharge. Eye infections can be serious in babies under one month old and may lead to problems if not treated quickly. Early care is essential to protect your baby’s sight and health.
Newborns receive antibiotic eye ointment at birth to help prevent serious eye infections, which can escalate quickly in babies less than a month old.
Take your newborn to the doctor right away if you see any of these eye infection symptoms:
- Redness or swelling of the eyelids: Can be a sign of infection or blocked tear ducts.
- Eye discharge: Yellow, green, or thick pus-like discharge could be a bacterial infection that needs immediate treatment.
- Eyelids stuck shut: If crusting around the eyes happens after naps, it can signal infection.
You may also notice that your newborn squints or turns away from light, has a fever, or is irritable.
One possible diagnosis is neonatal conjunctivitis. This eye infection, often caused by bacteria acquired during birth, can lead to corneal ulceration and blindness if untreated. Prompt evaluation and antibiotics are essential.
Consulting with a doctor is the best way to care for your newborn and ensure healthy eyes now and in the future.
When to take infants and older children to see a doctor for an eye infection
Take infants over two months old and older children to the doctor if their eye infection doesn’t improve in a few days, gets worse, or affects their vision. Signs like swelling, thick discharge, pain, or light sensitivity may need medical care to prevent complications and help your child feel better.
Pediatric guidelines show that many warning signs in newborns also apply to older infants and children. Doctors should evaluate any eye infection that doesn’t improve with home care or comes with a fever or other whole-body symptoms. Pus-like discharge, especially with an ear infection, is another reason to seek care.
In rare cases, symptoms like fever, eyelid swelling, or eye pain may signal severe conditions such as orbital cellulitis, which can spread quickly and lead to vision loss or systemic illness.
If you notice these signs, don’t wait. Early treatment is vital to prevent the infection from worsening and protect your child’s vision.
When to use home care and monitoring if your infant or older child has signs of a slight eye infection
You might use home care if your child has mild eye redness, no pain, and clear or slightly watery discharge. Gently clean the eye and look out for changes. Call a doctor if symptoms last more than 1–2 days or get worse. For babies under two months old, always get help sooner.
You can care for mild eye infections at home if your child has:
- Slight redness in one or both eyes: Redness may be the start of a mild viral or allergic reaction that heals without medical intervention.
- No thick discharge (only watery tears): Watery eyes without pus are less likely to be a severe bacterial infection.
- No eye pain, swelling, or vision problems: Home care is usually safe if your child is comfortable and can see normally.
- There is no fever or other signs of illness. A normal temperature and good energy levels suggest the infection hasn’t spread.
Eye care for your child at home isn’t complex and only requires that you:
- Gently wipe the eye with a clean, warm, damp cloth: This helps remove crust or discharge and keeps the eye clean.
- Wash your hands before and after touching the area. Good hygiene prevents the infection from spreading to others or the other eye.
- Keep your child from rubbing or touching their eyes: Rubbing can irritate the eye more and spread germs.
- Do not use any drops unless your doctor says it’s okay: Some drops may not be safe or helpful without a proper diagnosis.
Watch closely for any changes and stay alert to worsening symptoms or new signs of infection. Call your doctor if things worsen or don’t improve in 1–2 days. Early treatment can help avoid problems and protect your child’s vision.
Signs it’s time to see a doctor for an eye infection
See a doctor if the eye is red, painful, swollen, or has thick yellow or green discharge. Other warning signs include vision changes, light sensitivity, or fever. If symptoms don’t improve in a few days or worsen, it’s time to get medical help.
See an eye doctor right away if you exhibit any of these symptoms:
- Redness that spreads or persists: Persistent or worsening redness may indicate bacterial or viral conjunctivitis, or more serious conditions like uveitis. Uveitis is inflammation of the middle layer of the eye. Uveitis can be serious and may lead to vision loss if untreated. Signs that you have uveitis include redness, blurred vision, eye pain, floaters, or light sensitivity. Autoimmune diseases or injury cause uveitis. Steroid eye drops or pills reduce inflammation. If you have these symptoms, seek prompt medical evaluation.
- Blurry vision: Blurriness can signal corneal involvement, swelling, or deeper infection. Any vision changes associated with eye discomfort require prompt evaluation.
- Moderate to severe eye pain: Discomfort beyond mild irritation could point to corneal abrasions, keratitis, or other serious issues.
- Foreign body sensation: Feeling like something is in your eye, even if nothing is visible, can signal corneal damage or an embedded particle. Such sensations may indicate more serious infections like keratitis.
- Continuous or excessive itching: Itching may be allergy-related, but also occurs in viral or irritant conjunctivitis.
- Thick, colored discharge (yellow, green, or white): Such discharge suggests bacterial infection, especially if it causes lashes to stick together.
- Swelling of eyelid or around eye: Puffy lids, especially if red and painful, may signal periorbital or orbital cellulitis — both severe conditions.
- Sensitivity to light (Photophobia): Photophobia can accompany more serious infections like keratitis or iritis.
- Floaters or flashes of light: Floaters can be benign or may indicate endophthalmitis, an infection inside the eye that needs urgent attention. Eye infections like these can lead to vision loss.
- Decreased or sudden vision loss is always a red flag, potentially indicating a corneal ulcer, optic nerve involvement, or internal infection.
- Eye trauma or recent surgery: Infections following injury or surgery, such as LASIK or cataract surgery.
If you have severe symptoms like those noted here, like vision loss or intense pain, see your doctor immediately for an accurate diagnosis and appropriate care. Your eye doctor will likely perform a slit-lamp evaluation. A slit-lamp examination helps assess eye structure and health. It particularly examines the cornea, lens, iris, and the thin, transparent membrane that lines the inside of the eyelids and covers the white of the eye. It’s a key tool for diagnosing and monitoring eye diseases and conditions.
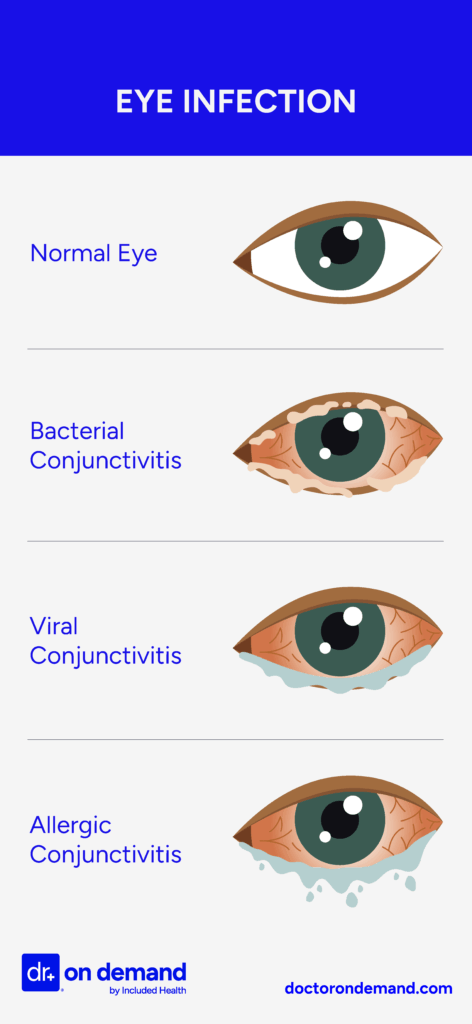
Types of eye infections
Eye infections can be bacterial, viral, or fungal. Doctors check your symptoms, look at your eye with a special light, and may test eye discharge in a lab to find the cause. Knowing the type of infection helps the doctor choose the proper treatment, such as antibiotic or antiviral drops.
Here are some of the different types of infections caused by bacteria, viruses, or fungi:
- Bacterial eye infections: Harmful bacteria can enter the eye and cause infections. Infection can happen from touching your eyes with dirty hands, using old makeup, or not cleaning contact lenses properly.
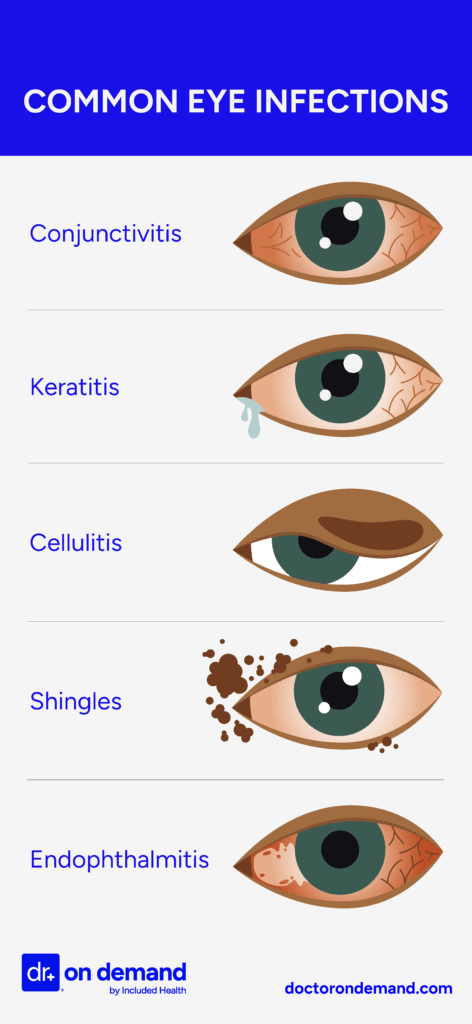
- Bacterial conjunctivitis (pink eye): Pink eye shows up as redness, swollen eyelids, pus-like discharge, crusting of the eyelids, and eyelids that stick together, especially after waking. Pink eye is very contagious and affects people of all ages. According to a 2024 research article titled “Conjunctivitis,” the infection is a common complaint in emergency departments, urgent care clinics, and primary care clinics. The authors write, “In the United States, this imparts a substantial economic burden on the healthcare system, costing about $857 million annually.” Antibiotic eye drops or ointments are the preferred treatment for pink eye.
- Bacterial keratitis: Symptoms include eye pain, redness, blurred vision, photophobia (light sensitivity), and discharge. It is often associated with contact lens wearers and requires prompt antibiotic treatment to prevent corneal damage.
- Blepharitis: Itchy, swollen, and red eyelids and a crust at the eyelid margins are signs that you may have blepharitis. If necessary, this condition is often chronic and managed with good hygiene and antibiotics.
- Endophthalmitis: Symptoms include severe eye pain, vision loss, redness, and swelling. This eye disease is a medical emergency and often occurs after eye surgery or penetrating eye injury. It requires immediate intravitreal antibiotics.
- Orbital cellulitis: Symptoms include painful eyelid swelling, fever, impaired eye movement, and vision loss. This severe infection of the tissues surrounding the eye requires hospitalization and intravenous antibiotics.
- Stye: Also known as hordeolum, the symptom of this infection is a painful, red lump on the margin of the eyelid. This infection is usually self-limiting; warm compresses can aid healing.
- Trachoma: Symptoms include chronic conjunctivitis, eyelid scarring, and the potential for blindness. It is the leading cause of infectious blindness worldwide and is prevalent in areas with poor sanitation.
- Viral eye infections: Viral eye infections are caused by viruses, like the ones that cause flu or cold, and are often painful. They spread by touching your eyes after coming into contact with someone with a viral illness, and coughing or sneezing.
- Herpes simplex keratitis: Also known as ocular herpes, symptoms include eye pain, redness, tearing, photophobia, and blurred vision. It can cause corneal ulcers, and antiviral medications are required to treat this infection.
- Herpes zoster ophthalmicus: Symptoms include a painful rash on the forehead and eyelids, redness, swelling, and eye pain. The virus affects a nerve in the face that connects to the eye. Antiviral medicine is needed to treat it and prevent serious problems.
- Viral conjunctivitis: Symptoms include redness, watery discharge, itching, and a gritty feeling in the eye. It is often associated with upper respiratory infections. While the disease is highly contagious, it typically resolves on its own.
- Fungal eye infections: When fungi get into the eye, usually from touching the eyes with dirty hands or through injury, you can end up with an uncomfortable or even dangerous eye infection. A 2024 study, “Immune Mechanisms of Filamentous Fungal Keratitis,” found that fungal keratitis is severe and “leads to more than 1.5 to 2 million new cases of complete vision loss or unilateral blindness each year.” This disease exists in different countries worldwide, and while rare in the U.S., all cases are serious. More common in tropical developing countries, it proliferates where filamentous (organisms that grow in long, thread-like structures) fungi live, and the plant matter gets into the eyes.
- Fungal keratitis: Symptoms include eye pain, redness, blurry vision, light sensitivity, tearing, and discharge. Fungal keratitis often relates to eye trauma, especially trauma that involves contact with plant matter, contact lens use, and eye surgery. Early treatment is essential to prevent vision loss. Treatment includes antifungal eye drops, oral antifungal medication, or surgery if medications don’t work or the cornea is badly damaged.
- Fungal endophthalmitis: Symptoms include decreased vision, eye pain, floaters, redness, and swelling. This fungal eye infection can happen after eye surgery, systemic fungal infection, IV drug use, or immunosuppression. Treatments include antifungal injections into the eye, oral antifungals, and sometimes surgery.
- Candida endophthalmitis: Symptoms include blurry vision, floaters, dull eye pain, or redness. Candida endophthalmitis infects the bloodstream, especially in hospitalized or immunocompromised patients. Treatment can be oral or intravenous antifungals and antifungal injections in the eye(s) if the infection is inside the eye.
- Ocular blastomycosis: Symptoms include vision changes, eye inflammation, and floaters and is often linked to a severe fungal infection caused by breathing in fungus spores. This infection usually starts in the lungs and can spread to other body parts, like the skin, bones, or eyes. Treatment includes systemic antifungals, taken in pill form. Patients may need long-term therapy and specialist eye care.
- Ocular coccidioidomycosis: Symptoms include eye pain, blurred vision, floaters, or possible retinal damage. This disease relates to lung infection, a common ailment in the southwestern U.S. that frequently spreads to the eye. Treatment includes oral antifungal medications. Eye inflammation may also require steroid eye drops under close monitoring.
- Ocular Histoplasmosis Syndrome (OHS): Symptoms include painless vision loss, central blind spots, and floaters. OHS may result from a previous lung infection, which leads to scarring near the retina. There is no cure, but monitoring is essential. Special eye injections may be used if abnormal blood vessels form in the retina.
Mild viral infections may only need monitoring, but bacterial and fungal infections almost always require medical care. It’s safest to have an eye doctor evaluate the problem when in doubt.
High-risk groups for eye infections
Contact lens wearers, diabetics, immunocompromised people, and individuals recovering from injury or eye surgery are at higher risk for eye infections. Sharing makeup, touching eyes with dirty fingers, and practicing poor hygiene also increase eye infection risk.
People at high risk for eye infections include:
- Contact lens wearers: Increased risk due to potential for corneal abrasions, improper lens cleaning and storage, and overwear, all of which can introduce bacteria, viruses, or fungi.
- Immunocompromised individuals: Weakened immune systems (due to conditions like HIV/AIDS, cancer treatment, organ transplant medications) make them more susceptible to various infections, including those of the eye.
- Dry eyes: Insufficient tear production can compromise the eye’s natural defense mechanisms, making it easier for pathogens to adhere and cause infection.
- Inflammation of the eyelids (Blepharitis): Chronic inflammation can disrupt the normal tear film and create an environment conducive to bacterial growth.
- Young children: Tend to touch their eyes frequently and have developing immune systems, increasing their risk of contagious infections like viral conjunctivitis.
- Diabetics: Higher blood sugar levels can impair immune function and blood flow, potentially increasing the risk and severity of eye infections.
- Individuals with recent eye surgery or injury: The protective barrier of the eye is compromised, allowing for easier entry of infectious agents.
- People using certain eye medications (e.g., steroid eye drops): Can suppress the local immune response, increasing susceptibility to infection.
How doctors treat eye infections
Depending on the cause, doctors treat eye infections with specific medications or procedures. Doctors use antibiotic, antiviral, and antifungal eye drops or pills to combat infections. Some infections need special hygiene. If the infection is critical or affects deeper eye parts, strongermedicine or surgery is the way to preserve vision.
Doctors have a wide variety of treatments available to treat eye infections, based on the type and severity of the condition:
- Antibiotic eye drops: Commonly used for bacterial conjunctivitis and some bacterial corneal infections.
- Antibiotic ointments: Can be used for bacterial conjunctivitis, especially in children, as they may be easier to apply. Ointments can temporarily blur vision.
- Oral antibiotics: Prescribed for more severe bacterial infections like orbital cellulitis or when the infection has spread beyond the surface of the eye.
- Antiviral eye drops: Used to treat viral infections like herpes keratitis.
- Oral antiviral pills: May be prescribed for more severe or persistent viral eye infections.
- Antifungal eye drops: Used to treat fungal keratitis. These infections can be challenging to treat and may require prolonged therapy.
- Oral or IV antifungals: Used for severe fungal infections like endophthalmitis or orbital cellulitis.
- Steroid drops: May be used in conjunction with antibiotics or antivirals to reduce inflammation, but they require careful monitoring by a doctor as they can sometimes worsen certain infections.
- Warm compresses: Often recommended for styes to help reduce swelling and promote drainage.
- Cool compresses: May provide comfort for viral conjunctivitis.
How Doctor On Demand can help with your eye infection
Doctor On Demand connects you with a licensed provider by video to check symptoms like redness, swelling, or discharge. They can diagnose common eye infections, recommend treatment, and send prescriptions if needed. It’s a fast, easy way to get care without leaving your home.
During your visit, the doctor will ask about your symptoms, when they started, and if you’ve had any eye injuries or use contact lenses. You can show your eye on camera, and the doctor may guide you to gently pull your eyelid or move your eye to help with the exam.
How to prepare for your Doctor On Demand visit for an eye infection
Before visiting Doctor on Demand, write down your symptoms and when they started. Take a clear photo of your eye. Have a list of any medicines or eye drops you use. Make sure you’re in a well-lit room. Be ready to answer questions and show your eyes during the video call.
Use this list to prepare for your Doctor On Demand video consultation:
- Write down your symptoms: Note when they started, whether they affect one or both eyes, and if symptoms are worsening. Symptoms to look for are redness, discharge, pain, swelling, or vision changes.
- Describe your discharge: Be ready to explain the color, amount, and texture of the eye discharge, such as whether it is watery, thick and yellow, or thick and clear. This information helps distinguish viral from bacterial causes.
- Check your vision before the visit: Cover one eye at a time and read something at arm’s length to note any vision changes.
- List any recent exposures: Include close contact with someone with pink eye, recent cold or flu, swimming pool use, or use of shared cosmetics or towels.
- Mention contact lens use: If you wear contacts, tell the doctor your brand, wearing schedule, and when you last changed lenses or solution. Stop wearing them before the visit.
- Take clear photos of your eyes: Take a close-up of each eye from the front and side in good lighting. These help the doctor assess swelling, redness, and discharge.
- List current medications and allergies: Eye drops, antihistamines, or recent antibiotics.
- Prepare your medical history: Note any past eye infections, surgeries, allergies, or chronic conditions like diabetes or autoimmune disorders.
- Ensure good lighting and internet connection: Sit near a window or a bright lamp. Have a mirror or helper nearby to assist during the exam.
- Know your pharmacy information: Be ready to confirm your preferred pharmacy so you can get your prescriptions quickly.
Doctor-answered eye infection FAQs
Have questions about eye infections? You’re not alone. Doctor on Demand providers answer common questions about symptoms, treatment, and when to get help. Learn what to expect during a virtual visit and how to prepare so you can get the proper care from home.
These are common questions people ask about eye infections:
- Should you go to the doctor for pink eye?
Most cases of viral pink eye go away on their own. But you should see a doctor if your eye is very red, painful, or if your vision changes. See your doctor if symptoms last more than 7–10 days. If a baby under 1 month old has pink eye, get medical help immediately. It could be serious.
- Can you go to your regular doctor for an eye infection?
Yes. Primary care doctors can treat common eye infections like pink eye. They can give medicine or send you to an eye specialist if needed.
- Can you see an optometrist for an eye infection?
Yes. Optometrists are trained eye care professionals who diagnose, manage, and treat eye conditions, including vision problems. They can treat many eye infections. They can prescribe and refer you to an ophthalmologistfor serious issues.
- What doctor should you see for an eyelid infection?
Start with your regular doctor or optometrist. See an eye doctor if it gets worse, keeps coming back, or doesn’t get better with treatment.
- How does a doctor diagnose whether an eye infection is bacterial or viral?
Doctors look at your symptoms and ask questions. Thick, pus-like discharge usually means bacterial infection, while watery discharge often means viral disease. Viral pink eye frequently shows up when you have a cold. Sometimes, doctors test the eye discharge in a lab to see if the infection is severe or unusual.
- Do you need a doctor’s prescription for eye infection treatments?
Yes. You need a doctor to prescribe antibiotics or antiviral drops. Some over-the-counter drops can help with symptoms, but won’t cure infections that need medicine.
- Can you self-treat an eye infection?
Mild viral pink eye often gets better with home care. Use warm compresses and artificial tears to make yourself more comfortable. Keep your hands clean and don’t share towels. See a doctor if your symptoms don’t get better in a few days or get worse.
- Can pharmacists prescribe antibiotic eye drops?
In some places, depending on local laws and agreements, they can.
- Do you need to see a doctor for conjunctivitis?
While mild cases may resolve on their own, you should consult your doctor if symptoms are severe, if you have significant pain, or if your vision changes. If the condition does not improve within a few days, visit the doctor. If the patient is a newborn or immunocompromised, see a doctor immediately.
About the authors

Quan Lam is a copywriter with over 15 years of experience writing and editing content for both start-ups and legacy brands, as well as 2 years of writing experience exclusively within the healthcare space. She currently lives and works in New York City.

Dr. Jeanette Carpenter is board certified in Family Medicine and practices in Virginia. She has an interest in preventative medicine and holistic medicine and has a certification in plant based nutrition from eCornell. She believes stress and lifestyle impacts the disease process and spends extra time educating patients on lifestyle modifications that can improve their overall health.



